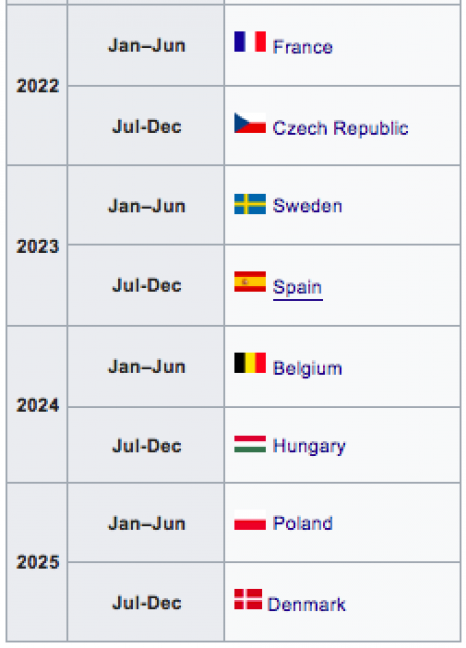
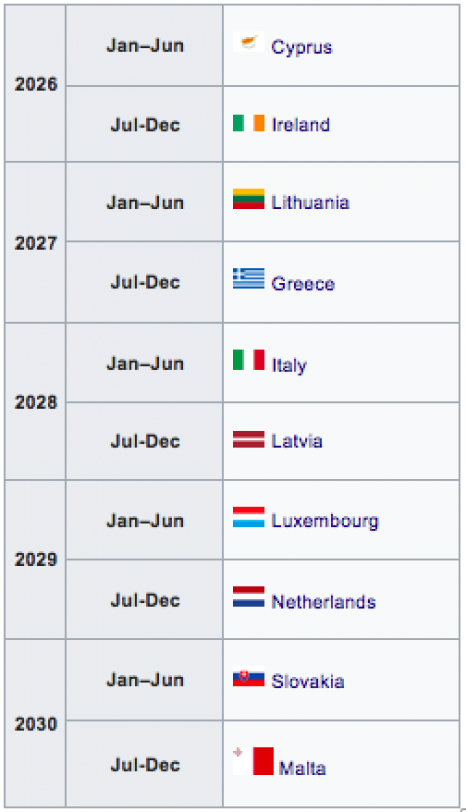
BREXIT: What now for universities?
Briefing of EUA gives more information.
With courtesy from the European University Association EUA.
On 31 January 2020, the UK has left the European Union. Many in the university sector are committed to the European idea and regret this fact, and there is widespread worry about how this will affect the strong links in research, education and innovation between the UK and the rest of Europe. However, having avoided a chaotic “no-deal” Brexit allows for clarity about the next steps in the negotiation and about the new relationship between the UK and the EU. This briefing gives an overview of what has already been agreed and the further process towards the future relationship between the EU and the UK, with a focus on areas relevant to universities.
Brochure can be downloaded here
_w490_h170_1.png)
_w490_h528_1.jpg)
_w490_h566_1.jpg)
EFPA participates in EU-funded project: RECOVER-E
In this interview, Laura Shields-Zeeman, Head of the Department of Public Mental Health and Prevention at Trimbos Institute, the Dutch Institute for Mental Health and Addiction talked to Anne Leybina, EFPA Executive Council Liaison officer about the RECOVER-E project, an EU funded research and implementation project for community mental health in Europe.
By: Anna Leybina
1. What is RECOVER-E?
The overall goal of RECOVER-E is to implement and evaluate an evidence-based community-based service delivery model for recovery-oriented care in five sites in middle-income countries in Europe (Bulgaria, Croatia, Montenegro, North Macedonia, Romania) to improve the level of functioning, quality of life, and mental health outcomes for people with severe and enduring mental ill health. RECOVER-E is a European Commission Horizon 2020 project with 16 partners in 11 countries; the project complements numerous ongoing efforts in mental health service delivery transformation and innovation in Europe.
2. What are the expected outcomes and benefits of the project?
Specific objectives include:
- designing, implementing, and evaluating recovery-oriented care, and including peer experts in community mental health teams;
- identifying intervention and program elements, as well as contextual factors, which enhance sustainable implementation of community-based mental healthcare; and
- developing evidence-based care pathways and treatment protocols for regional and national decision-makers.
Read the full interview here below
To read the full interview, scroll down within this block.
Some benefits of the project include:
- creating the conditions in regions/cities where service users have access to improved care that supports recovery;
- creating an evidence base that supports and facilitates the implementation of community mental health services;
- leveraging content expertise to navigate local factors that affect system reform, and to share the positive work being done in the project with key stakeholders
3. What are the key messages from this project?
RECOVER-E is a three-and-a-half-year Horizon 2020 research initiative funded by the European Commission, bringing together 16 partners from 11 countries in Europe to drive transformations in mental health service delivery for people with severe mental illness. It aims to stimulate good practices in community-based mental health care to serve the needs better of people with severe mental illness.
4. What is the ideal destiny of the project results after it is over?
Ideally, the project would contribute to a society in which service users have access to improved care that supports recovery. Second, the project would contribute to putting a foundation in place to continue offering and paying for the delivery of community-based mental health services by multidisciplinary community mental health teams.
5. What would be the financial and psychological benefits of Recover-e project and its’ possible applications? Why can’t we leave mental health care system as it is now in those countries?
With respect to the financial benefits: It’s still too early to discern what the economic benefits of the project’s intervention are. But we are currently collecting data to inform a health economic evaluation that will show back both the budget impact of introducing a community mental health service into the system as well as the cost-effectiveness of the intervention compared to care as usual in each of the five sites.
As for the psychological benefits: Focusing on recovery goals and care goals of patients and working towards that collaboratively, providing care where the patient wants it (e.g. via home visits, in public places like a café or public garden, in the clinic). In some countries without a decentralized mental health care system, people with severe mental illness are repeatedly admitted and discharged from hospital because there are no appropriate community alternatives. This cycle of re-hospitalization does not facilitate social integration and functioning, or recovery, which further affects quality of life. Care delivery through community mental health teams enables clients to work on their recovery across various aspects of life while participating and building/maintaining bonds within their communities.
6. How is the project engaged with community mental health leaders?
The site leaders in the five implementation sites are community mental health champions in their own settings and in Europe and are not only involved in local community mental health initiatives at the policy and clinical level, but also in other parts of Europe. Several project partners are also leading and members of other community mental health initiatives in Europe, such as the EuCOMS network.
Visit EUCOMS website
7. What kind of specialists are involved in the project (and from which countries)?
In each of the five implementation sites, there is a research team and a community mental health team. The community mental health team is staffed by a mix of psychiatrists, psychologists, nurses, social workers and peer workers (i.e. persons with lived experience of a severe mental illness). Outside of the 5 implementation countries, we have consortium partner organizations from 6 other countries that include service user organizations (peer specialists), implementation science experts, health services researchers, clinical specialists and trainers, professional associations for psychologists and psychiatrists, and think tanks dedicated to policy and practice change in mental health and addiction care.
8. How are mental and public health institutes involved? What organizations are involved?
As mentioned above, the RECOVER-E consortium includes a large complementary mix of partners including clinical mental health services that have gone through similar transformations in their service delivery approaches as the 5 RECOVER-E project sites are going through now. In our consortium we have academic institutions, think tanks for mental health and addiction, service user organizations, professional associations, and public health institutes involved. Public health and mental health institutes are involved in the 5 sites in both the delivery and evaluation of the intervention, which are the multidisciplinary community mental health teams.
9. How are you planning to get better policy impact?
Having policy impact through our work will require a combination of efforts. First, it is important to map out the current decision-makers in each site and gauge their support towards mental health services development. Then, each site has made a policy influencing strategy which specifies one key policy ask related to mental health services development, around which a targeted action plan is formulated to engage decision-makers. Finally, two policy dialogue sessions (one in the beginning and one of the end) bring together national and regional stakeholders country to discuss priorities, evidence gaps, and project results needed to contribute to sustaining service delivery transformations made throughout the duration of the project.
10. How psychology and EFPA are involved? How can we benefit and contribute?
Psychologists are a crucial part of the community mental health teams and in working with service users towards achieving their recovery and treatment goals. EFPA is an important partner in the dissemination of the project findings and lessons learned, specifically by raising awareness of these service delivery changes and lessons learned with national professional associations of psychologists both in the RECOVER-E implementation sites and beyond. Part of the process of deploying a new service delivery model for severe mental illness in these 5 sites has involved a needs assessment and situation analysis of the current mental health system in each site, as well as an extensive training and mentoring program. Ultimately, our hope is that these training materials and tools for monitoring developments in mental health care are institutionalized and embedded in ongoing professional associations in each of the 5 sites, a process which EFPA plays an important role in facilitating.
11. Which practices can be implemented in other countries?
Multidisciplinary community mental health teams are already active in many countries throughout Europe and globally. We have evidence that they work and in many settings are preferred as a service delivery approach by service users. Countries that are currently working to reform or improve their mental health care systems may benefit from understanding, tailoring, and adopting various practices and processes taking place in RECOVER-E (for example in relation to implementation or policy influencing processes and strategies).
12. What are “mobile teams”? Are there similar interesting findings or initiatives that can be used?
Mobile teams are multidisciplinary community mental health teams that deliver care to people with severe mental illness such as schizophrenia, bipolar disorder and severe depression. The teams consist of a mix of professions like psychiatrists, psychologists, peer workers, social workers and nurses, in order to provide holistic care that takes into account the service user’s social, personal and clinical context and recovery goals into account. Such teams operate within mental health services in many countries globally and in some well-resourced systems, there are even specialized community mental health teams (e.g. forensic assertive community treatment teams, specialized treatment teams for dual diagnosis, etc).
13. What are the workpackages? Who are workpage leaders and what’s the difference between the packages? Are they implemented similarly in all the three countries?
Work packages are essentially sub-components of work in the project, or represent a certain theme of work in a project. Work package leaders are representatives from a number of the 16 consortium partners, who meet regularly in the form of the project’s management team and discuss progress and issues ongoing in each of the work packages. Some of the work packages are more general and cut across the whole project (e.g. Work Package 1 which is Overall Management and Coordination, and Work Package 7, Dissemination) versus other work packages which are really content focused and focused on efforts to support work in the 5 RECOVER-E sites (e.g. WP3 which is implementation support or WP6, Bridging the gap between Policy and Practice). All Work Packages are implemented across the 5 countries in a similar method.
Where can we find more information about this?
More information about the Work Packages can be found on our project website:
www.recover-e.eu.
14. How are the project results monitored and assessed?
We have a comprehensive evaluation approach within the project, which is currently ongoing. Let me share with you our specific research objectives:
- testing the impact of the intervention on patient outcomes and service utilisation outcomes;
- gathering in-depth data on implementation processes, which includes identifying key contextual factors, barriers, and facilitators of implementation; and
- assessing the cost-effectiveness of the intervention compared to usual care.
- The outcomes and results of the research on the community-based service delivery in the five sites will be shared with policymakers, stakeholders in Central and Eastern Europe, healthcare providers, and researchers through policy dialogues, conference presentations, briefings, reports, and journal articles.
In order to understand the processes of the teams and the impact on care, the work of the teams will be evaluated using a mix of research methods. First, five hybrid effectiveness-implementation trials have been devised (1 per trial site) to assess the effects of the teams and of the delivery of new team-based community mental health care approach on implementation outcomes (i.e. the coverage and fidelity of evidence-based care at the health system level) and on patient-level outcomes (i.e. health gains in terms of improved role functioning and better health-related quality of life). These five trials have a pragmatic, non-blinded study design; patients are to be randomised into two parallel groups: receiving new community-based versus receiving hospital-based mental health care. Alongside the trials, a health economic evaluation will assess the cost-effectiveness of the intervention compared to care as usual, as well as assess the net benefits of the intervention across the 5 trials. To evaluate implementation outcomes and identify intervention and contextual factors that enhance sustainable implementation of community-based mental healthcare, a qualitative process evaluation will be carried out.
15. How psychologists from Croatia, Romania, Bulgaria can learn more, participate, contribute?
As I mentioned before, psychologists are a key member of the community mental health teams and an important partner in delivering therapies and services in a way in which is supportive of the recovery journey and recovery goals of a service user. There are a few ways I think psychologists from the RECOVER-E sites can learn more, participate and contribute.
First, identify how a service delivery structure like a community mental health team delivering outreach care could be adapted for your setting or practice. What would need to change to make this way of working possible, and in what way would it help your clients? Second, what kind of professional development and capacity building opportunities would you need and how can you work with your national association for psychologists and local and national policymakers to advance these efforts? Third, this is an important networking opportunity for psychologists working in the RECOVER-E project to connect with their peers and share challenges and lessons learned from delivering care in a new way, which can lead to new synergies and opportunities in the mental health system going forward.
What is RECOVER-E?
RECOVER-E (LaRge-scalE implementation of COmmunity based mental health care for people with seVere and Enduring mental ill health in EuRopE) is a project funded by the European Union’s Horizon 2020 research and innovation programme under grant agreement No 779362.
EFPA is a partner in the RECOVER-E project
Read also the previous article on RECOVER-E published in the February 2019 edition of the EFPA News Magazine
_w1470_h644_1.png)
Image: RECOVER-E objectives. Source: www.recover-e.eu.
RECOVER–E workshops will be held at the following congresses:
- European Congress of Psychiatry Madrid
Workshop: Successes and Challenges in Advancing Community-Based Mental Health Care in Europe: Reflections from the RECOVER-E Project.
Importante notice: The EPA Congress has been rescheduled and shifted to July 2020. Workshop date to be confirmed.
- International Congress of Psychology Prague
Important notice: the ICP congress has been rescheduled to July 18-23, 2021

Parenting for a Digital Future newsletter
Read the latest edition here
At the beginning of a new decade, we take a look back at our recent posts from the end of 2019 and ahead to what is in store for 2020, including the publication of our book in June.
- Digital communication and family relationships
- Technology in schools: opportunities and risks
- Digital literacy and creativity
- Privacy and rights
- Mental health and wellbeing
- New LSE Media and Communications blog
If you are interested in finding out more about the work of the Media and Communications Department at the LSE, we have recently launched a new blog Media@LSE. The blog aims to promote critical research into the vital role of media and communications in contemporary society. Themes cover, but are not limited to: communication history, data protection, political communication, public service broadcasting, internet governance and children and the media. Source: London School of Economics and Political science: subscribe here
With courtesy of Sonia Livingstone – Professor of Social Psychology at the London School of Economics and lead investigator of the ‘Parenting for a digital Future’ research project.
Read also:
Also read previous article in EFPA News Magazine February 2019
The Top 10 Mistakes patients make in cross-broder healthcare
Every EU/EEA citizen has the right to receive both public or private health services in any other EU Member State, Iceland, Liechtenstein or Norway, and to enjoy assumption of all or part of the medical costs by the national health service or health insurance provider in the patient’s home country. Before making use of this right it is of great importance that patients inform themselves, are well-prepared, and know which mistakes to avoid.
The Directorate-General for Health and Food Safety of the European Commission just finished a new publication of a toolbox intended to help patients in getting to grips with their rights under the Cross-border Healthcare Directive.
The toolbox, comprising checklists, templates, manuals and FAQs, is available in all European languages and you are invited to disseminate the information via your channels as you see fit.
A tweet is also available on the toolbox, should you wish to retweet it

Download the leaflet directly
2020 Workplan Health Programme for EU citizens
Véronique Wasbauer, Director of the Consumers, Health, Agriculture and Food Executive Agency (CHAFEA) which manages the Health Programme for the European Commission, explains what are the key actions of 2020 work plan and what the Health Programme does for EU citizens. What will the Health Programme bring to you?
(1)_w676_h450_1.jpg)
First of all, what is the Health Programme?
The Health Programme supports EU policies in the area of public health: it provides financial support to EU-wide projects to improve public health, prevent illness and eliminate threats to physical and mental health in European countries. It also supports the implementation of EU legislation in the field of serious cross-border threats to health, tobacco control, cross-border health care, substances of human origin.
To date, the programme has funded 976 projects and actions, working together with 7387 organisations across Europe. The current Health Programme is the third one, running from 2014 to 2020.
And what is an annual work plan?
To put it very simply, the annual work plan outlines the actions Chafea will implement during the year and sets aside the necessary budget to carry them out, in line with the priorities set by the Commission.
What is noteworthy about the 2020 work programme?
2020 is the last year of the third Health Programme. The work plan will continue to focus on the following four objectives:
1. Promoting heath, preventing diseases and fostering supportive environments for healthy lifestyles,
2. Protecting Union citizens from serious cross-border health threats,
3. Contributing to innovate, efficient and sustainable health systems,
4. Facilitating access to better and safer healthcare for Union citizens.
Related topics:
EFPA’s involvement in the following Horizon 2020 funded EU Projects:

Mental Health Europe publishes Finnish Presidency Scorecard
MHE evaluates each Presidency’s commitment to and promotion of mental health by releasing ‘Scorecards’.
With courtesy of MHE
Source
What is the Scorecard about?
To engage with and to monitor the performance of the rotating Presidency of the Council of the European Union, MHE has devised a scorecard system. We use it to evaluate each Presidency’s commitment to and promotion of mental health. It is based on the following criteria:
- Promotion of mental health and well-being
- Commitment to the rights of persons with psychosocial disabilities
- The involvement and empowerment of users of mental health services

How successful was the Finnish Presidency (Jul-Dec 2019) in terms mental health & human rights?
The Finnish Presidency has notably made a commitment to promote the well-being in all policies. It made the “economy of well-being” one of its key priorities for its mandate.
Mental health and well-being were regular topics of discussions throughout the six-month mandate. The Presidency is leaving us with the concrete invitation to issue a European Mental Health Strategy.
While appreciating the efforts and commitment to bring mental health at the forefront of discussions in the EU agenda, users of mental health services where not consistently involved throughout the discussions.
We invite the Government of Finland to continue its admirable work to promote positive mental health, prevent mental ill-health and protect the rights of persons with psychosocial disabilities.
Download the Scorecard to find out more about the Finnish Presidency’s score

MHE launches a ‘Guide to personal recovery in Mental Health’
Mental Health Europe (MHE) launches a new resource for people experiencing mental health difficulties. A ‘Guide to Personal Recovery in Mental Health’ follows on from ‘A Short Guide to Psychiatric Diagnosis’ and is the second publication in a series of short guides.
This series aims to help people who have personal contact with the mental health system – either during or after receiving a diagnosis – to stay better informed. ‘A Short Guide to Psychiatric Diagnosis’ was produced for people who receive a mental health diagnosis. The ‘Guide to Personal Recovery in Mental Health’ aims to describe ways of thinking about, managing and overcoming mental ill-health.


Click here to download the guide

Download the full MHE-report 'MHAP Review 2017 - 2019' here
Blogs & newsletters
Here is a list of interesting blogs to follow and newsletters to subscribe to:
Clinical Psychology in Europe
Health and Care Professions Council (UK)
European Commission Public Health-EU: e-newsletter
International Association of Medical Regulatory Authorities (IAMRA)
European Parliament IMCO (Internal Market Committee)
United Kingdom: Professional Standards Authority (UK)
European Social Network ESN
Ireland: CORU Regulating Health + Social Care Professionals (Ireland)
Healthcare Professionals Crossing Borders HPCB


In person:
All over the European Union there are hundreds of Europe Direct information centres. You can find the address of the centre nearest you at: https://europa.eu/european-union/contact_en
On the phone or by email:
Europe Direct is a service that answers your questions about the European Union. You can contact this service:
by freephone: 00 800 6 7 8 9 10 11 (some operators may charge for these calls),
at the following standard number: +32 22999696 or
by email via: https://europa.eu/european-union/contact_en
EU publications
You can download or order free and priced EU publications here
Multiple copies of free publications may be obtained by contacting Europe Direct or your local information centre
EU law and related documents
For access to legal information from the EU, including all EU law since 1952 in all the official language versions, go to EUR-Lex at:
http://eur-lex.europa.eu

Open data from the EU
The EU Open Data Portal ( http://data.europa.eu/euodp/en)
provides access to datasets from the EU. Data can be downloaded and reused for free, for both commercial and non-commercial purposes.
(1)_w466_h334_1.png)