READ MORE
NEW: EFPA News Magazine Interview Section
EFPA is one of the 14 partners of the EU funded project H-Work Multilevel interventions to promote mental health in SME’s and Public Workplaces.
With this interview section in the EFPA News Magazine, we aim to keep our member associations informed about the progress in the H-Work project and to provide insight into the role of the different partners of the consortium. These interviews with project partners will become a permanent section. We hope it makes for a pleasant and informative read.
In previous editions of the News Magazine EFPA has informed about the H-Work project through articles in the editions of July 2020 and February 2021. We also referenced the first H-Work newsletter in the edition of November 2020 and published an interview with H-Work Coordinator professor Luca Pietrantoni.
In this edition, Jolien Vandeneynde interviewed Josefina Peláez Zuberbühler, one of the lead researchers at UJI and Richard Wynne, representative and contributor for ENWHP within the project.
H-WORK interview:
Dr. Josefina Peláez Zuberbühler
By: Jolien Vandeneynde
1. What is the role of your organization in the H-Work Project?
Universitat Jaume I (UJI) from Spain, is the leading partner of the Work Package (WP) 2 ‘CREATE’. This WP is the preparatory phase that creates the theoretical basis for the development of the H-WORK (assessment, intervention, evaluation) Toolkits. The objective is to integrate the H-WORK consortium expertise related to best practices, digital technologies, and EU policies in mental health promotion in Small and Medium Enterprises (SMEs) and public organisations. UJI also contributes to WP3 ‘COLLECT’, in implementing psychosocial risks assessment and defining and tailoring interventions to be implemented in each Spanish intervention site. Our past experience on evidence based positive psychological interventions lets us take an important role within WP4 ‘INTERVENE’. We coordinate the intervention phase in the Spanish intervention sites, ensuring the implementation of the multi-level interventions. Last but not least, UJI contributes to creating a dissemination plan, elaborating scientific publications in collaboration with other research partners in the project, and attending conferences and networking events.
-
2. What is your role within the project?
My main role is to coordinate the UJI team’s work in order to achieve our contributions in the different Work Packages. Specifically, co-coordinating the tasks related to the development of the theoretical framework for WP2, coordinating the preparatory and intervention phases in the Spanish intervention sites, contributing to the design and implementation of interventions, keeping active communication with the Spanish intervention sites (3 SMEs and one Public Hospital), and with the rest of the H-WORK consortium partners, and finally, contributing to dissemination activities and scientific publications.3. Can you present your team?
Our team in UJI is composed by members of WANT Research Team - Psychosocial Prevention and Healthy Organizations. All of them are psychologists specialized in the development of pioneering tools for the assessment and intervention of psychosocial health at work. Dr. Marisa Salanova is the director of the WANT team, and full professor in the area of Social Psychology at UJI. Within the project, Marisa is the leading researcher, in charge of supervising the UJI team. The rest of the team consists of Dr. Susana Llorens and Dr. Isabel Martínez, both associated professors in the area of Social Psychology, Dr. Cristián Coo Calcagni, senior researcher in charge of facilitating the implementation of the interventions within the project, Mabel San Román, PhD student contributing to the different project activities, and myself, coordinating UJI Team tasks and contributing to the different project activities.
To read the full interview, fold out:
4. What is the impact of COVID on the work of your organization for the H-Work project?
With regards to the communication within the H-WORK partners, the impact has not been so disruptive, given that most of the meetings from the very beginning were meant to be online. Unfortunately, we have not been able to join together in conferences, networking and continue the Consortium meetings face to face. We are really looking forward to it. Hopefully, the European Association of Work and Organizational Psychology (EAWOP) congress in Glasgow next year will be a good opportunity to get together and present interesting theoretical and practical results achieved in the project so far. One important setback that we have faced in UJI due to the Covid-19 pandemic was the drop out of two of the Spanish test sites (a small company and a big public hospital) before starting the preparation phase because of the important economic, health or psycho-social consequences suffered. Fortunately, we have just reached an agreement with two other similar organizations, and we are really looking forward to starting Needs Analysis activities this semester.Considering that mental health promotion at work is even more important nowadays due to the current crisis, we believe that our work within the project is not being greatly affected. In order to achieve the expected outcomes, some of the activities have been restructured, for instance the assessment and intervention protocols have been modified with the inclusion of COVID-19 issues, and we are innovating with digital solutions for the development of the meetings and intervention activities.5. What has your team accomplished in the project so far?
Our first accomplishment, in collaboration with Università di Bologna partners, has been the Deliverable 2.1 H-WORK Theoretical Framework. This deliverable gathered an in-depth analysis of the consortium expertise related to best practices in the workplace mental health promotion, integrated into the Individual, Group, Leader, and Organizational (IGLO) model, in addition to state-of-the-art digital technologies and services on the market. The deliverable also provides indications on how to incorporate gender, cultural differences, stigma and co-morbidities that are relevant to the design and implementation of the H-WORK Toolkits, and a summary of relevant EU and national policies on mental health promotion at the workplace. During the preparation phase, the H-WORK assessment tool has been tested throughout the analysis of the needs on two of the Spanish intervention sites. This Needs Analysis consisted of individual interviews to senior and middle managers and focus groups to employees aiming at identifying actions and interventions needed to improve mental health and wellbeing in the workplace. A series of multilevel interventions have been proposed and agreed for their implementation on the different test sites, such as a Positive Leadership Development, Strengths-based Micro-Coaching, Positive Stress Management, Positive Social Climate and Appreciative Survey Feedback. All of them are based on previously validated Positive Psychological Interventions studies. Together with Università di Bologna, Technische Universität Braunschweig, Universiteit van Amsterdam, and QED group from Czech Republic, we have participated in webinars with the objective of training the trainers of the different research partners to be aligned in the implementation of interventions in the different countries' test sites.6. What are you currently working on and what are the next steps?
Related to the Theoretical Framework deliverable, we are currently developing a series of joint publication efforts together with different members of the consortium. Also, together with Università di Bologna and the contribution of other members of the consortium, the innovation in digital technologies and updates on European policies are being constantly monitored and updated throughout the project. This will result in the development of a second Deliverable (D2.2) meant to be finalized by the end of the project. As a second step within the preparation phase, baseline data collection through quantitative questionnaires is currently being implemented in two of the Spanish testbeds as a Pre-intervention assessment. Two of our test sites are currently starting the implementation phase that will last until December of this year (2021). At the same time, the preparation phase with needs analysis activities is about to start in two other Spanish test sites.
7. What are currently the main obstacles for your work and for the project in general?
The first obstacle we had to deal with was the outbreak of the pandemic crisis due to COVID-19. This has led to some delays on starting the preparation and implementation phases in the different test sites, in addition to modifications to the Assessment and Intervention protocols. Despite these setbacks, data collection and implementation of the different actions are being developed without major drawbacks. I will say that one of the main difficulties or challenges in our work is to engage the different stakeholders in the test sites and find ways to motivate employees to participate. Today, more than ever, it is crucial to create awareness about the need to mitigate the consequences of the current pandemic crisis, such as psychological distress, burnout, depression, anxiety, social stigma, and to help them build resources and skills to achieve psychological healthier work environments.
8. What are your expectations regarding the outcomes of the project for your country?
With the exploitation of the H-WORK assessment, intervention and evaluation toolkits we expect to contribute to the creation of psychosocial healthy workplaces. Public organizations and SMEs often have insufficient knowledge and resources to manage workers' mental health and well-being effectively. In order to address this difficulty, we seek to provide technical guidance on good practices and procedures to establish policies that can reduce occupational exposure, stress and risk reduction; and promote well-being of workers, especially in SMEs and public environments. To this end, identifying and providing best practice evidence based multilevel interventions within the project, would be crucial to orientate future actions for these types of organizations. At both the national and European levels, the main challenge of the project is to support organisations and their representatives in recognizing psychosocial risk factors, adopting measures and providing further innovative products and services to effectively promote mental health in the workplace, along with policy recommendations for employers, occupational health professionals and policy makers.
9. How do you think your organization and EFPA can collaborate in the H-Work Project?
We are honored to work with the leading European Federation of Psychologists Associations (EFPA) in the project. EFPA is one of the greatest contributors to Work Package 2, specifically in gathering relevant European policies and regulations related to mental health promotion in the workplace. Our next challenge within this Work Package is the monitoring of such European policies, together with the provision of recommendations and strategies for policy makers, tasks that will be possible because of the crucial alliance with the EFPA Standing Committee of Work & Organisational Psychology.H-WORK interview with European Network for Workplace Health Promotion - ENWHP
Dr. Richard Wynne
By: Jolien Vandeneynde
1. What is the role of your organization in the H-Work Project?
Our role is mainly confined to dissemination of project progress and results through our network of members and newsletter recipients. We are also involved in making our expertise in relation to workplace health promotion and workplace health and safety available to the project. We have considerable policy experience in the area at national and EU level and we are also making this knowledge available to the project.-
2. What is your role within the project?
Managing the ENWHP contribution. Specifically:- Contributing expertise on policy in EU
- Contributing experience of workplace health promotion
I also take part in the various management and WP meetings of the project. In general, I try to bring to bear a knowledge of the realities of workplaces to the more theoretical work of the project.
3. Can you present us your team?Our team is a flexible one, drawn from our Board Members and from the secretariat of the ENWHP. Contributors to the project to date have included:
- Dr. Richard Wynne, Work Research Centre, Ireland
- Dr. Maria Dolores Sole, INSHT, Spain
- Prof. Giuseppe Masanotti, Department of Public Health, University of Perugia, Italy
Between us, we have many decades of experience in the area of workplace health promotion and workplace health and safety. Our backgrounds include Occupational Medicine and Organisational Psychology.
To read the full interview, fold out:
4. What is the impact of COVID on the work of your organization for the H-Work project?
Very little – we are a virtual organisation and apart from a commitment to attend project meetings we have seen little impact on our working methods. At Work Research Centre, where I am a Director, the impact has been largely confined to work in Ireland, where due to travel restrictions, it has proved impossible to make site visits etc. However, virtual meetings have largely replaced these and the impact on working methods has not been too severe.
5. What has your team accomplished in the project so far?
To date we have contributed expertise in relation to European policy on Workplace Mental Health Promotion and methods of implementing workplace health promotion. We have also been involved in disseminating project information through our network.
6. What are you currently working on and what are the next steps?
At present we are involved in updating our communications about the project to our network on our website, social media and newsletter. We will also be involved in reviewing Deliverables from the project, the next one being due over the course of the next month or two.7. What are your expectations regarding the outcomes of the project?
It is difficult to say at present as the project is still in development mode. I would hope that a set of proven and practical interventions to promote mental health at work will result, but there are many variables that can affect such an outcome over which the project has limited control. Already the Covid pandemic has resulted in delaying the implementation of field trials and it will continue to affect their implementation as the project progresses (e.g. homeworking populations, the need to have online support etc.). Beyond this major issue, there are the usual workplace factors to be considered, e.g. levels of support by workplace actors, levels of need in the workplace, identification of workplace champions, overcoming unforeseen obstacles and so on.
8. What are currently the main obstacles for your work in general and in the project?
I think the main obstacle is the difficulty of establishing working relationships with the project team. ENWHP are not central to the development or the implementation and evaluation work of the project and establishing working relationships with appropriate partners has proved difficult in the absence of face-to-face meetings. Hopefully, travel restrictions will be lifted in the near future and this barrier can be overcome.9. What is the biggest strength of your organization in advancing the project or helping other partners?
I think our strengths lie in practical experience of implementing workplace health initiatives, workplace mental health policy at national and EU level and in disseminating project information.
10. How do you think your organization and EFPA can collaborate in the H-Work Project for WP2 and WP7?
I think it may be possible to develop a joint strategy to these WPs as we occupy somewhat similar roles within the project. I would be interested to hear what EFPA thinks on this issue.
Comment from EFPA:
As mentioned EFPA and ENWHP have indeed similar roles within the project. EFPA is very interested in the opportunity and willing to collaborate with the ENWHP on providing effective communication and dissemination strategies for the project. We look forward to establishing and maintaining a good working relationship with the ENWHP and to creating a joint strategy.Back to top
February 2021
H_WORK refers to new online tool that helps employees stay motivated during corona lockdown.
A new online training tool developed at the Eindhoven University of Technology TU/e helps workers to be happier, more motivated, and better performing in the home office.
The COVID-19 pandemic has changed our lives. Long work commutes, the office cubicle, and gossip by the coffee machine have been replaced by a home office where work is intertwined with our daily lives. This is a challenging situation for many and can lead to impaired well-being. To help workers develop skills needed to navigate this trying period, TU/e researcher Evangelia Demerouti has developed an online training program, which is available for all to use for free until July 2021. And initial tests show that workers who followed the training were happier, more motivated, and performed better in the home office.
If you want to access the tool and follow the 4-week training program, you can access it via this link
The course is in Dutch.(Source )
H-WORK and EFPA
H-WORK consortium brings together broad multi-disciplinary expertise that unites the leading knowledge in the field of occupational health, methodology, policy development and communication, while at the same time provides additional expertise in advanced technologies and innovation. EFPA is partner in this EU project (2019-2023) which has received funding from the European Union’s Horizon 2020 research and innovation programme under grant agreement No 847386.
Publication recommended by H-WORK:
'Development and validation of the coaching-based leadership scale'
Read more under recommended publications in this edition Back to top
Being a Psychologist in Recover-E: Romania
In our previous issues, we have conducted interviews with psychologists involved in the Recover-e project and shared their experience. This time, EFPA EC member Anna Leybina asked colleagues from Romania a few questions that would help to understand the nature of psychologists’ work in Recover-E in their country._w430_h158_1.png)
-
How has the RECOVER-E project been received in Romania?
Raluca: This project is new for our country, as well as the concept of community mental health teams (CMHT). Because our mental health system is mostly institutionalized, this idea of mobile community mental health teams hasn’t been implemented before. For us it was very interesting to try a new way of working. And we knew from other countries that people are pleased with this approach when different specialists provide them support within the community. So, we, as specialists, were very interested to see how this concept would work being implemented here in Romania.
How have the CMHT’s been received in your organisation/hospital?
Tiberiu: Community mental health teams’ operation is an extension of our practice, as well as it goes in line with our ethos and philosophy of work. As an institution, we already were community oriented. Now we have more tools and methods focused on community mental health and the needs of our patients (beneficiaries). So, on one side it was a challenge, but on the other – because we had an a lot of experience as a team, it was very interesting to learn together the new ways of working with our beneficiaries in community, not hospital environment.
Fold out to read the full interview.In your view how do the CMHTs contribute psychologically to service users with severe mental illness?
Raluca: Support is important for every person, as for every human being. The idea is the support is delivered in our beneficiaries’ regular settings in the form of diverse mental health needs satisfaction. It is important for every human being to know that if you are alone in your house, there will be someone available to support you, especially if that someone knows how to provide support in a proper way. So from psychological point of view such support is really important.
How are psychologists involved in the project?
Tiberiu: I think psychologists play an important role in CMHTs, because we contribute to the methods used as both of us are trained in clinical psychology, CBT and motivational interviewing. Psychologists can be useful in at least two ways. The first one, the psychological issues and solutions they identify for patients and psychological information we provide to patients and their families; the second one, psychologists put the team together as psychiatrists and social workers can always discuss their work with psychologists, who are liaising with the whole team expertise. So, psychologists serve the patients and the team.
Raluca: Even though psychiatrists have a long history of being central in the treatment process, over the time due to education, practical examples, overseas experience, many of our citizens understand the importance of psychologist in dealing with diverse mental health issues. Protocols for depression indicate psychotherapy for mild and moderate episodes as first line of intervention. Psychologists have an essential role in the treatment of mental health issues. So the role of psychologists is increasing.
Who are the psychologists involved in the CMHT? What was the selection process?
Raluca: As for qualification, it is definitely important, but the key is to love your profession and strive to implement your skills and knowledge in the best way possible. Any effort you make for professional development will contribute to your work.Tiberiu: Clinical expertise is definitely important, but we also see the need in community expertise. And Recover-E project helps in gaining more community experience.
Raluca: There was a selection to this project in a sense. We both worked in the mental health area for a number of years, starting from the scratch, e.g. by introducing the idea of mental health in the 90’s which was new for Romania. Since then, we are trying to develop the area and to participate in diverse projects. Over the long period we have started and developed quite a number of projects, and were somehow visible for the Recover-E consortium then they were looking for the partners.And why have you chosen to be the part of this project?
Raluca: There are five countries which are now implementing this project. So, it was interesting to see how it would be implemented here in Romania. Would this work in the same way as in Eastern Europe as it works in the Western ones? Would it be beneficial for our patients?Tiberiu: I guess for every professional, e.g. nurses, not only psychologists, it is important to move out of the classical clinical settings into community settings. And it is also the need of the beneficiaries. So, it was a very obvious step.How is the collaboration between different professionals organised in the CMHTs?
Raluca: Our team consists of one psychiatrist, two nurses, two psychologists, one social worker, and two peers. We are very lucky as we work with our colleagues in a very natural and easy way. There are divided responsibilities, but no one is acting without communicating with the other members of the team. E.g. social workers, they possess some information we don’t have, hence we listen to her suggestion regarding the support provided to a particular patient.
Tiberiu: we’ve been working together with our colleagues for a long time and mental health is a multidisciplinary area. Without medical input, without social input there won’t be such progress. Only together we can improve the life of our beneficiaries. If there is someone, we are answering to it is our beneficiaries. We are telling them if we se some positive developments in their state.
Raluca: As psychologists’ work, Tiberiu is mostly involved with patients’ needs, and he supports them in the way they request which is initially directed to the whole team. I work mostly with the team members to discuss the ways they execute their duties and do things, the ways to improve that. As these two aspects come together very often, there is no clear line “it is my work, and this is yours” we are just trying our best to provide professional input.
What is the process of work with your patients?
Tiberiu: Because we’ve been working in this classical clinical environment for so many years, we knew most of the patients before the project started because it is intended for chronical conditions. As all other colleagues are in the hospital at least once a week we meet together, and invite peer-workers too, to discuss concrete needs of our patients. Of course now due to Covid-19 we use computer and phone more to communicate with our team and our patients.Do you connect with psychologists from other RECOVER-E sites to exchange experiences and idea for your work as a psychologist?
Raluca: Because the project is built in such a way that each of us has some responsibilities and we lead a certain workpackage, I had an opportunity to visit colleagues in two countries: North Macedonia and Bulgaria to learn about the work of my colleagues there. Implementation meetings happen every month where we discuss the way things are going in each site of the project and exchange practices. So, we know that this model of community mental health is implemented pretty in much the same way across the five countries with some cultural adjustments, of course.Tiberiu: It was very easy and beneficial for our team to communicate with other teams. We received the training, the same one as was received by the others so it is very easy to communicate with them as we have the same background.What is your role and responsibilities in the CMHT? How big is your caseload? Do you share your tasks with other members of the CMHT?
Tiberiu: As case managers we have 15 cases, but as psychologists we are involved in every case which requires psychological input. We share tasks with the social worker or with the psychiatrist as the psychiatrist is not always available. But we share these tasks due to good communication in our CMHT and with our colleagues. For example, then the beneficiary needs a change in medication or doesn’t have an idea on which medications would be required, then we invite psychiatrist to provide education on why it is important to take this medication. Or with social workers: when beneficiary needs to prepare papers for local administration and doesn’t know how to do that and the social worker is not available, we are assisting in this matter. At the beginning we support peer-workers to make them feel confident.What does a day in your working life look like now you are working in the community mental health team (CMHT) if you compare it to what it looked like before the project?
Tiberiu: The day starts with the meeting where we go through cases, we think need more support. There we establish the best ways to interact both with the patient and with the team. For example, we see that making the home visit in Romania is a very formal event, the beneficiary may be stressed by the fact that a big group of people visiting their house which might not be ready (not clean enough or else), so we’ve found that there is a need to identify one or two people within the team who will visit the patient. Or if we need to meet elsewhere, e.g. a park or a cafeteria. These arrangements that are not happening in the professional institutional environment are very effective.
Raluca: we have a number of cases as case managers, so we calling the beneficiaries to check on their state: e.g. the challenges they are facing, their daily routine. We need to ask more questions to reveal hidden issues as usually the answer to the question “How are you?” is “I’m fine”. So we need to identify if this “fine” is justified or if we have to consider the situation in a bit more details. We have patients who are staying well, and those, who are not. For example, the prescribed medication doesn’t work well anymore. So, after those calls, we discuss with the team the cases that need some intervention as other team members might have more information on the case, e.g. the social worker as she deals with all the patients helping to apply for social benefits she may have additional information. And if we identify the need in additional intervention we identify, who is the most suitable to deliver this intervention. Or we send the team member who interacted with a patient more so gained the trust, to identify the issues and collect information. So basically, the task of the day is to collect information and to discuss with the team in the next few days the cases that require more attention.Before we were working only with the patients admitted in the hospital, there was nothing provided beyond the hospital work. And now CMHT’s work is a continuation of what is going on in the hospital.How did you experience shifting from a focus on problem/symptoms of the patient to recovery oriented method of delivering care?
Raluca: It is not easy, as many of them do not know what to do with their life, how to adapt in the society, as they were told before that they are ill and the only thing, they needed to do was to take care of their sickness. And many patients have to learn on how to open opportunities for their life, or how to find a company to drink coffee or to play chess.
How do you focus your approach towards recovery?
Raluca: once the patients make a few steps and see that they can do more, they start trusting themselves. We start with them with minor steps to strengthen their self-esteem.What changes do you see – using a recovery oriented care approach among patients?
Tiberiu: Before the project clinical environment was very safe for both, the professionals and the patients. Patients came, told their symptoms, stayed in the hospital till they got better and the they left the institution. And that was the end of the interaction. But now through this project we are really recovery oriented. The goal is not to get better in the institution, but in the environment, they came from, to feel secure and empowered in their regular settings, to have the life they want to have. It’s not the goal they can achieve alone, it is the goal we have to achieve together. We have to draw the recovery path through the community, to find points that can help to follow the path and get better.
Raluca: We can’t expect that a person with 20 years of schizophrenia would suddenly reintegrate professionally, but for such person to socialize and to go together for a holiday is a real achievement. So, recovery orientation means a better quality of life.How is your work different now during COVID than before the pandemic?Raluca: It is not very easy as “human touch” is relatively minor in digital interaction. On the other hand, we need to teach ourselves self-support in such circumstances as many social interactions and habits are on pause. So, we help each other to identify new sources of energy. And then we teach others and share our experience.
Tiberiu: There is a positive side as our patients needed to learn how to use online environment. Also, if before they could visit the hospital if they feel worse, now they have to think twice due to the risk of being infected. So they learn to interact digitally and it is the real gain in the long run as they need to acquire new skills to perform regular tasks (e.g. getting a medical prescription in a new way). It wasn’t easy for them, but they have to learn that there are other ways of communication. Also, they now need to be more proactive in calling their doctor to report on their state or to ask for help. We did a series of trainings for them on how to use their smartphones or to use zoom meetings.
Raluca: The patients now are calling to us just to talk and by that we understand that the patient might need more attention and we communicate that to our team members.What are your insights from participation in this project? Is there any important information you’d like to share with your colleagues around Europe or in your country?
Tiberiu: The training we received was very useful. It was also interesting to work with our peer-colleagues as the energy of the team has changed. They also help us to identify patients’ strengths to build the recovery process. Another thing is that professionals have to be aware of the cultural settings, e.g. for home visits in Romania which oblige the host to be prepared, so professional has to ensure that visiting beneficiary’s house is not a stressful event, but a helpful event. And the visitor has to be a relevant visitor, not just anybody from the team.How has this experience changed you professionally?
Raluca: It was definitely professionally developing as it is a new way of work and we had to adapt and improve ourselves in some areas. We communicate more, to share tasks, to educate ourselves a bit more. Community team work is not very easy, but very rewarding as we see the progress in our beneficiaries.Tiberiu: It was very helpful to feel that there is always someone around you in the team who can give you extra resources. Also, it is something we previously saw only in books now we see it live: if the patient becomes more active his or her recovery becomes more successful. Clinical stings make patients more passive while community settings make them more active.Back to top

Mental Health Europe is hosting the second edition of the European Mental Health Week from 10 – 16 May, 2021.European commission – Directorate General for Health and Food Safety
"Mental health and the pandemic: living, caring, acting!" is a one-day, virtual event along five themes - understanding – living – caring – responding – acting to highlight the mental health impact of COVID-19, Monday 10th May 2021.
The event will bring together a wide array of speakers, including representatives from EU countries, the European Commission, European Parliament as well as from patient organisations, non-governmental organisations, health professionals, civil society and international organisations. The conference language will be English. Participation and registration is open to all.
About the event
What does it mean to live in a world defined by COVID-19 and to provide care in this pandemic age? This one-day, virtual event during the European Mental Health Awareness Week 2021 aims to highlight the mental health impact of COVID-19 along five themes - understanding – living – caring – responding – acting – by:
- giving a voice to those affected
- illustrating what it means to live in a world defined by COVID-19; looking at the situation of different groups in our society, including people with pre-existing mental health problems and those providing care
- sharing examples and promising practices
- exploring what we know and what we need to understand better
- discussing how to ensure that our health systems are well-equipped, now and in the future

2021 European Mental Health Week: Daily
May 10, 2021
May 10th marks the start of 2021 European Mental Health Week. This year’s theme ‘Mental Health Matters’ puts a spotlight on mental health as a high-profile societal issue as well as a deeply personal experience for everyone during these challenging times.
Over a year of pandemic, lockdowns and coronavirus restrictions have put a strain on many people’s mental health. We are all experiencing a different pandemic. Some experience the loss of a loved one, miss friends or family, others lost their workplace security and feel lonely, stressed and uncertain about the future. Now more than ever, mental health matters.
Join Mental Health Europe and its members from across Europe for various events, discussions, and activities during the week. From high-level policy webinars to conversations and live sessions on social media – there is something for everyone.
We want to focus on sharing advice and support and encouraging people to talk about all aspects of mental health and how they cope with difficulties and look after their own wellbeing.
Learn more about the week Back to top
_w438_h298_1.png)
Source: Website Council of Europe, Commissioner for Human Rights.
The commissioner for human rights calls for urgent mental health service reform. Reform of mental health services: an urgent need and a human rights imperative.
Dunja Mijatović, the Council of Europe Commissioner for Human Rights, took a stand against human rights violations in mental health care and called for urgent reforms.
‘Mental health reform is an extremely challenging task for all our member states, given the complexity of the issues and the huge gap between agreed international standards and the reality on the ground. This, however, makes it all the more urgent. Let us turn the current challenge of the pandemic into an opportunity by thoroughly transforming mental health services in Europe, with human rights as our guide and compass,’ urges the Commissioner.
Back to top
European Pain Forum
EFPA is a member of European Pain Forum, which is organized by EFIC/European Pain Federation.
By: Borrik Schodt, member of EFPA Standing Committee on Psychology and Health.
There are 13 members of the Forum, and the first official meeting was in Spring 2019. As members of the Forum, we participated in making a revision of opioid practice recommendations: /
Professor Kevin Vowles at Queen’s University Belfast, School of Psychology, did a great job representing EFPA in the revision of the paper.
This is an important work. We have learned from USA that a liberal opioid-prescribing practice can result in opioid-misuse and serious problems for many people: In USA overdoses involving opioids killed nearly 50,000 people in 2019, and 38 persons died of overdose from prescribed opioids every day.
We have also learned that the reversal of a liberal practice can result in people in need of pain-relief not getting necessary help. We need to prevent a transition from opioid-epidemic to opioid-phobia. One of the means to achieve this are evidence-based guidelines or recommendations.
The opioid paper gives recommendations for when and how opioids should be used. The paper also states that non-pharmacological interventions should be the first choice. Non-pharmacological interventions are in large a not-defined concept – including strategies ranging from exercise, to psychotherapy and warm baths. Psychologists should contribute more to this, by describing how to relieve pain or cope with pain, using psychological strategies – including relaxation techniques, hypnosis, preventing catastrophizing, give the patient a sense of control, distraction, acceptance, etc.
Back to top
-
European commission proposes action to uphold child rights and support children in need
April, 2021
Source: Website EU commission, EU Strategy on the Rights of the CHILDThe Commission has today adopted the first comprehensive EU Strategy on the Rights of the Child, as well as a proposal for a Council Recommendation establishing a European Child Guarantee, to promote equal opportunities for children at risk of poverty or social exclusion. In preparation of both initiatives, the Commission, in association with leading global child rights organisations, collected the views of over 10,000 children.
EU Strategy: six thematic areas & proposed action
1.Children as agents of change in democratic life
2. The right of children to realise their full potential no matter their social background
3. The right of children to be free from violence
4. The right of children to child-friendly justice
5. The right of children to safely navigate the digital environment and harness its opportunities
6. The rights of children across the globeThe new European Child Guarantee
In 2019, almost 18 million children in the EU (22.2% of the child population) lived in households at risk of poverty or social exclusion. This leads to an intergenerational cycle of disadvantage, with profound and long‐term effects on children. The European Child Guarantee aims to break this cycle and promote equal opportunities by guaranteeing access to a set of key services for children in need (under 18 year olds at risk of poverty or social exclusion).Under the European Child Guarantee, it is recommended to Member States to provide free and effective access for children in need to:
- early childhood education and care – for example, avoid segregated classes;
- education and school-based activities – for example, adequate equipment for distance learning, and school trips;
- at least one healthy meal each school day; and
- healthcare – for example, facilitating access to medical examinations and health screening programmes.

European Parliament calls on Member states to adopt the Child Guarantee as a matter of priority
April, 2021
The European Parliament, in collaboration with the EU Alliance for Investing in Children, calls on the Council of the EU and its Member States to implement the European Pillar of Social Rights, to adopt the Child Guarantee as a matter of priority and ensure that the Child Guarantee starts being implemented 6 months from the adoption of the Recommendation.
Back to top
Brexit:
Recognition of professional qualifications
Find here updates regarding the negotiations between the EU and UK:
Additional draft text for the Agreement on the New Partnership with the United Kingdom 7 September 2020 (recognition of professional qualifications). EFPA will keep you informed on this matter.
This document is the European Union's (EU) proposal for the EU-UK FTA. It has been tabled for discussion withthe UK. The actual text in the final agreement will be a result of negotiations between the EU and the UK.
Blogs & newslettersHere is a list of interesting blogs to follow and newsletters to subscribe to:
Clinical Psychology in Europe
Health and Care Professions Council (UK)
European Commission Public Health-EU: e-newsletter
International Association of Medical Regulatory Authorities (IAMRA)
European Parliament IMCO (Internal Market Committee)
United Kingdom: Professional Standards Authority (UK)
European Social Network ESN
Ireland: CORU Regulating Health + Social Care Professionals (Ireland)
Healthcare Professionals Crossing Borders HPCB


In person:
All over the European Union there are hundreds of Europe Direct information centres. You can find the address of the centre nearest you at: https://europa.eu/european-union/contact_enOn the phone or by email:
Europe Direct is a service that answers your questions about the European Union. You can contact this service:
by freephone: 00 800 6 7 8 9 10 11 (some operators may charge for these calls),
at the following standard number: +32 22999696 or
by email via: https://europa.eu/european-union/contact_en
EU publications
You can download or order free and priced EU publications here Multiple copies of free publications may be obtained by contacting Europe Direct or your local information centre

EU law and related documents
For access to legal information from the EU, including all EU law since 1952 in all the official language versions, go to EUR-Lex at:
http://eur-lex.europa.eu
Open data from the EU
The EU Open Data Portal ( http://data.europa.eu/euodp/en)
provides access to datasets from the EU. Data can be downloaded and reused for free, for both commercial and non-commercial purposes.(1)(1)_w510_h196_1.png)
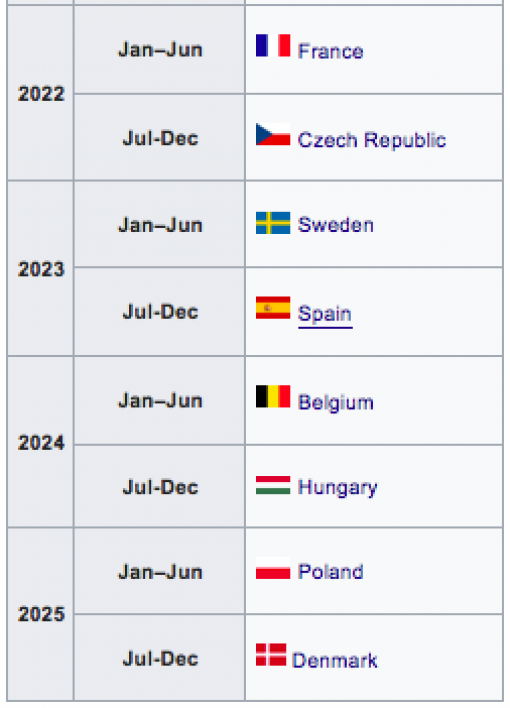
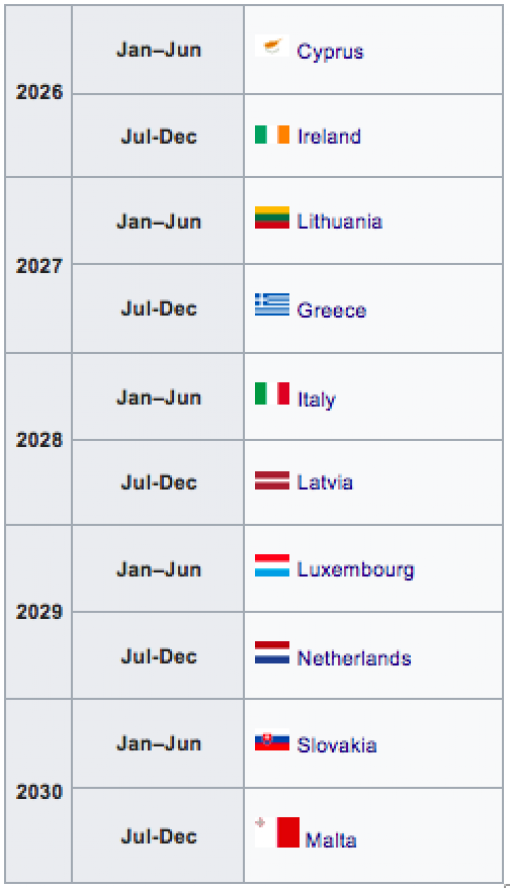
Back to top
-
_w306_h378_1.jpg)

_w328_h452_1.jpg)
_w512_h176_1.png)
_w1460_h796_1.png)
_w460_h158_1.png)
(1)_w692_h480_1.jpg)
(1)_w654_h462_1.jpg)
_w1462_h814_1.png)

_w672_h400_1.jpg)